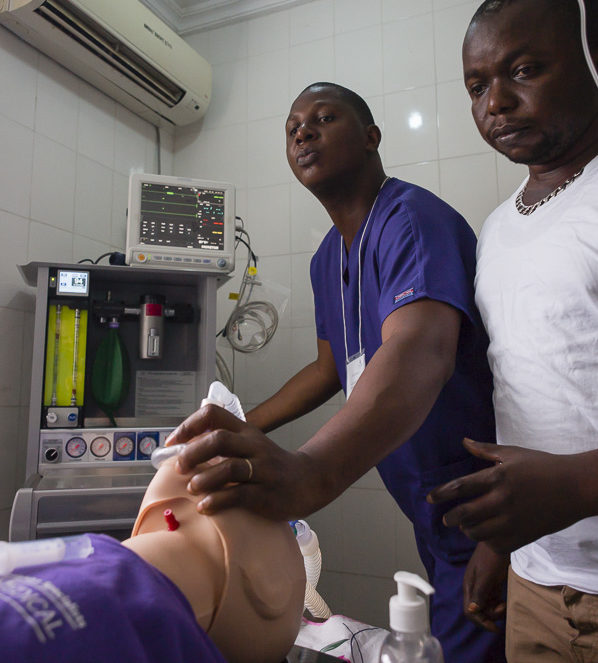
National UAM Installation & Training in Sierra Leone: An Interview with Dr. John Sampson



In October, Gradian worked with the Sierra Leone Ministry of Health and Sanitation to install UAMs at every public hospital in the country. To ensure that each hospital could deliver anesthesia confidently, we sponsored the Johns Hopkins University School of Medicine to conduct a month-long clinical training course on inhaled general anesthesia and patient management for the country’s nurse-anesthetists. Taking a decentralized “train the trainers” approach covering Sierra Leone’s four provinces, the course resulted in more than 50 newly trained anesthesia providers and a sustainable training environment to support the country’s revamped surgical capacity. Hopkins will be hosting a refresher course in 2017 to assess the skills and knowledge of the trainees.
Here’s an interview with Dr. John Sampson, Associate Director of Global Surgical Care at Hopkins, who oversaw the training:
Q: What was the purpose of the training, and why was it so important?
Dr. Sampson: Surgery in Sierra Leone is a major challenge. The country is severely limited in the procedures it offers due to a lack of general anesthesia and provider training. Anesthesia in Sierra Leone is most commonly delivered through ketamine injections, which are easier to administer than other forms of general anesthesia and solve for the country’s shortage of viable equipment (almost all anesthesia machines are either broken or unused). However, ketamine is a suboptimal alternative for general anesthesia and would never be used in the US as the sole anesthetic agent.
My team and I at Johns Hopkins had recently completed a project to introduce the UAM to Sierra Leone, paying particular attention to infrastructure and human resource needs that it had to meet. Unlike other machines we’ve seen, the UAM stood up against the shortages of oxygen, electricity and biomedical technicians, so we knew it was a good fit. The problem was that Sierra Leone’s nurse-anesthetists never had reliable access to an anesthesia machine and the patient management it requires. So we developed this course at Gradian’s request to complement the Sierra Leonean government’s purchase of UAMs for their public hospitals.
Q: How was the training carried out?
Dr. Sampson: I sat down with my research coordinator, Dr. Howard Nelson-Williams and Sierra Leone’s two anesthesiologists, Dr. Michael Koroma and Dr. Eva Hanciles (retired) to brainstorm a sustainable training environment that enables the confident use of anesthesia equipment and patient management. We landed on a identifying six dynamic nurse anesthetists from around the country whom we’d train to be our local trainers, eventually leading decentralized trainings in each of Sierra Leone’s four regions. We developed several simulation models with “breathing” intubation mannequins so the trainees could see various scenarios in real time. The simulations were intensive, interactive and iterative as the students’ skill level increased.
In the first week we trained the trainers at KCM Hospital in Freetown through a combination of didactic lectures and by simulations on airway management and the effects of halothane (one of the UAM’s anesthetic drugs). During the second week the trainers led a training session at the regional hospital in Makeni with mentoring from Dr. Koroma, Howard and me. In the following two weeks the trainers ran courses in Bo and Kenema with minimal and declining guidance from us until they were fully qualified to train on their own. In the end we trained 50+ anesthesia providers, accounting for more than half of Sierra Leone’s provider community. We hope to raise funding to train the rest.
Q: Did you witness anything during the course that stood out – challenges, successes, unforeseen circumstances?
Dr. Sampson: Having been a part of similar projects in the past, I knew that unforeseen challenges were to be expected. In this case, we anticipated oxygen and power shortages posing problems, so we pre-stressed the course design to ensure that we were prepared for infrastructure failures. This meant changing our curriculum slightly to encourage anesthetists to counsel their surgeon counterparts on the UAM’s capabilities in failure mode.
I was amazed to see how well the project went overall – both because of and in spite of the challenging environment. Specifically, one trainee from Connaught Hospital acknowledged, “I feel so much more confident intubating and monitoring patients now.”
Q: How did you plan to measure the training’s success, and was it successful by those standards or did you have to change course?
Dr. Sampson: The initial success of the training was borne out during the training itself – having the opportunity to work with trainees in a repetitive manner (drills lasted 2-3 hours) was rewarding for all parties involved. But the real test will come during annual refresher courses administered by the Sierra Leone Ministry of Health and Sanitation (MOHS), beginning in February 2017 – we will get a chance to see how well the trainees have retained their skills and knowledge, and we’ll be able to document that data alongside what’s actually happening in the country’s operating theaters, which will be the ultimate measure of success.
Success will also hinge on the MOHS’ commitment: the Ministry made a major investment in anesthesia equipment, so now it must protect that investment by ensuring that other pieces are in place for it to pay off, such as backup oxygen, voltage stabilizers and halothane (not to mention the technicians necessary to service the and support the equipment). We are also hoping they will start an anesthesia residency program at the national medical school.
Q: What can Sierra Leone do now that it couldn’t do before the training?
Dr. Sampson: In short, each of Sierra Leone’s public hospitals can now offer more and safer surgical procedures than they could previously, bringing much-needed care to the millions of patients they serve. For instance, before the training, it would have been dangerous to operate on a trauma patient with a full stomach without the training we provided in rapid induction anesthesia, or on a woman giving birth with high blood pressure since ketamine causes blood pressure to rise. But now, anesthetists have the ability to intubate patients properly and administer halothane safely, overcoming both of those challenges. Plus, with the UAM, they can do this whether or not they have reliable oxygen or electricity.
Q: Are there any lessons from the training that you’d like to relay to the broader global surgery community?
Dr. Sampson: The main lesson I would note is that training can’t happen in a vacuum: training design must account for the difficulty of the situation and the limitations of the context. At the end of the day, Western trainers need to ask themselves: would you accept what you’re advocating for? If you’re pushing for ‘task-shifting’ in a low-income country, would you go under the knife with a nurse-anesthetist who might not have guidance from a doctor?
I’ve also found that it’s better to focus on one country – really zeroing in on its challenges so it can actually make strides – than the box-ticking approach that many training organizations take.